Living With End-Stage COPD
You hear the term “end-stage chronic obstructive pulmonary disease (COPD),” and realize this is a very serious lung disease. COPD is the third-leading cause of death in the United States and a significant cause of disability.
However, the term “end-stage” is somewhat misleading, as it’s not always the last stage before death.
In medical terms, "end-stage" refers to the last treatment stage for a progressive disease. The goals of care then change to providing comfort. Some people may be gravely ill. But many are taking very good care of themselves - healthy diet, regular exercise, taking prescribed medications.
The Global Initiative for Obstructive Lung Disease (GOLD) has described four stages of COPD:
- Stage I - Mild COPD
- Stage II - Moderate COPD
- Stage III - Severe COPD
- Stage IV - Very Severe COPD
The last stage of COPD indicates a person with significant shortness of breath even when resting. At this stage, you are at high risk for lung infections and respiratory failure.
Several factors determine your life expectancy at Stage IV. Your smoking history, the severity of shortness of breath (dyspnea), fitness and nutritional status are all factors in whether you are very sick or living a fairly normal life.
What Is COPD?
Let’s take a step back to examine the condition known as COPD. COPD is a progressive disease, as it gets worse over time if there is no treatment. While doctors can’t cure the lung damage or the COPD, they can prescribe medications that improve symptoms and prevent complications.
Symptoms of End-Stage COPD
A person with end-stage COPD is likely to have severe symptoms, including:
- A chronic cough
- Sudden worsening, of the condition
- Frequent phlegm production
- Difficulty finishing a meal due to shortness of breath
- Low blood oxygen levels
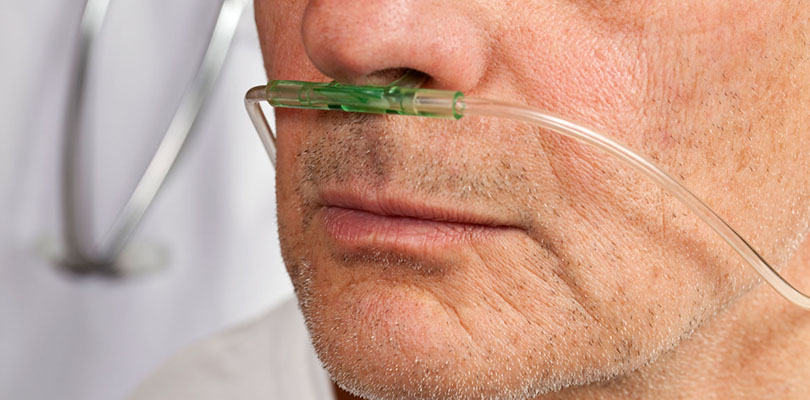
- Need for oxygen on a regular basis
- Shortness of breath with mild activity (a short walk)
The goals for COPD treatment are to prevent the disease from progressing to end-stage COPD.
Treatment for COPD
When a person develops end-stage COPD, they must take steps to prevent worsening symptoms – as each flare can further damage the lungs, slowing down recovery.
To reduce the risk of flares:
- Quit smoking.
- Avoid secondhand smoke in all forms, including clothing that smells like smoke.
- Check outdoor air quality, avoiding exposure on smoggy and heavy pollen days.
- Get a pneumonia vaccine and flu shot.
It’s also important to see a doctor immediately for signs of infection, like fever and yellow or green-tinged sputum.
COPD and cold weather do not go well together, but that does not mean you have to suffer. Here are some ways to tame the symptoms.
Treatment for End-Stage COPD
Surgery is an option for some people, including lung transplant surgery. According to the Cleveland Clinic, about 43 percent of people getting a single-lung transplant survive the 5-year mark. A person must meet certain criteria, and there must be a compatible donor.
Beyond that, your doctor may prescribe the following treatments:
- Bronchodilators. If you have shortness of breath during regular activity, short-acting bronchodilators may be prescribed. If that isn’t effective, your doctor may prescribe a long-acting bronchodilator as well.
- Inhaled glucocorticoids. Patients with severe breathing difficulty and COPD flares may need this.
- Oxygen. Oxygen (via an oxygen tank) reduces breathlessness when if you have low blood oxygen levels.
- Opiates. Morphine is effective in improving shortness of breath. However, only a small number of patients get morphine due to serious side effects.
- Noninvasive Positive Pressure Ventilation (NIPPV). This therapy may improve shortness of breath and reduce retention of carbon dioxide, but only in certain circumstances.
Therapies and counseling that can help:
- Pulmonary rehabilitation. This therapy helps all COPD patient at every stage of this disease.
- Nutrition counseling. Malnutrition is a significant risk for people with end-stage COPD and greatly increases the risk of death.
- Social and emotional support. Support helps people live longer, healthier lives despite COPD. Many people also benefit from this support to help them deal with end-of-life issues.
- Complementary therapies. Relaxation techniques may help relieve shortness of breath. Visualization, meditation, massage, and music therapy (with instruments, radio, or CD) are all useful.
Living Without End-Stage COPD
If your COPD has not advanced to end-stage, you can take steps now to prevent its progression. A healthier lifestyle will help you stay in good health.
- Stop smoking. Smoking is the pathway to COPD, and smoking cessation programs are very effective at helping people finally kick the habit. There’s no better way to improve your health and well-being - and slow the progression of COPD - than to quit smoking forever.
- Physical activity. A daily walk is the next best way to improve your health and longevity. Regular mild exercise is good for your lungs and your overall health.
- Change your diet. Healthy eating is critical to improving your health. You will feel better, including more energetic, and fight infection better. Good nutrition is the basis for healthy living.
- Be optimistic. Even though you have a chronic illness, you can learn to cope with it. Get the support you need from family and friends. Talk to your doctor, your minister or to a psychologist. Focus on creating a healthy life for yourself, so you can enjoy the years ahead. End-stage COPD isn’t the end.